New Syphilis Test May Be What Is Needed as Incidence Continues to Rise
As data emerges showing that syphilis rates are up yet again, the FDA has granted a waiver allowing a rapid test for the infection to be conducted in doctor’s offices, clinics, emergency rooms, maternity wards, and other non-laboratory settings. Experts hope that access to immediate results can increase both treatment and prevention and stem the tides of this growing epidemic.
In December, just days before the Centers for Disease Control and Prevention (CDC) announced increased rates of primary and secondary syphilis, the Food and Drug Administration (FDA) granted a waiver allowing a rapid test for the infection to be conducted in doctor’s offices, clinics, emergency rooms, maternity wards, and other non-laboratory settings.
Experts hope that access to immediate results can increase both treatment and prevention, and stem the tides of the growing epidemic.
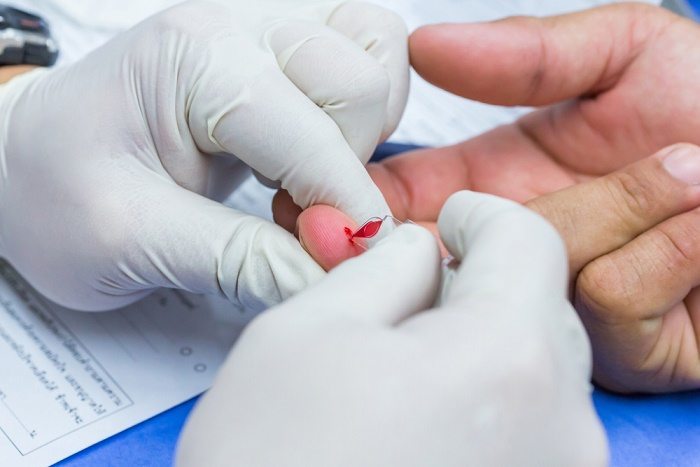
The rapid syphilis test, called Syphilis Health Check, requires a finger prick of blood and can provide results in 12 minutes. It was approved by the FDA in 2011, but was categorized as being moderately to highly complex. This meant that it could only be used in certified laboratory settings.
In order to be used in other settings where it could provide patients and providers with quick answers, the test needed to receive a CLIA (Clinical Laboratory Improvement Amendments) waiver. The waiver essentially states that the test is simple enough to be conducted by those without laboratory experience.
The FDA granted the waiver after the manufacturer demonstrated the test was accurate and easy to use. The agency reviewed blood sample data taken from 417 test subjects collected at non-laboratory testing sites such as doctor’s offices. The tests were performed by 12 people who had not been trained on how to use it and the results were accurate, even with these untrained operators.
Syphilis, a sexually transmitted disease caused by the bacterium Treponema pallidum, leads to small, round, painless sores called chancres, which can appear on the external genitals and anus, as well as inside the vagina and rectum. Sores can also appear on the lips and in the mouth.
Syphilis is transmitted through direct contact with these sores during sexual activity as well as from mother to newborn during childbirth.
There are three stages of syphilis. The primary stage, which occurs within ten days to three months after infection, is usually characterized by the appearance of one sore. The sore typically lasts three to six weeks and goes away on its own. Without treatment, the disease progresses to the secondary stage. This phase often starts with a rash that appears on one or more parts of the body.
It can also cause lesions on mucous membranes, fever, swollen lymph glands, sore throat, patchy hair loss, headaches, weight loss, muscle aches, and fatigue. Because these symptoms are so common with other ailments, syphilis is sometimes called the “great imitator,” and many who are infected do not realize it.
If left untreated, syphilis can proceed to the latent stage, which can last as long as ten to 20 years. During this time, a person may have no visible symptoms, but the disease can be damaging to the brain, nerves, eyes, heart, blood vessels, liver, bones, and joints. Signs and symptoms of late stage syphilis include difficulty coordinating muscle movements, paralysis, numbness, gradual blindness, and dementia.
At one point, rates of syphilis were so low in the United States that it looked like the disease was on the verge of eradication. In 1999, when just 6,657 cases of primary and secondary syphilis were reported, the CDC announced an elimination campaign designed to work with states to wipe out the disease. The number of syphilis cases has grown since the end of the 1990s, especially among men who have sex with men.
The CDC last month released data for 2013 that revealed there were 17,375 cases of primary and secondary syphilis that year. This represents a 10 percent increase over 2012 and comes on top of an 11 percent increase between 2011 and 2012. Almost 75 percent of cases were seen in men who have sex with men.
Prompt diagnosis and treatment during the primary and secondary phase—which are the most contagious—is important to prevent long-term health consequences and to prevent further spread of syphilis. Until now, however, testing for the disease has required blood to be sent to a laboratory, which means patients leave the clinic without either a diagnosis or treatment.
“We know from almost a decade of using rapid HIV tests how important it is for patients to get a test and a diagnosis in the same visit,” William Smith, executive director of the National Coalition of STD Directors (NCSD), told Rewire. “This means they can be connected to care and support immediately, that they don’t continue to unknowingly spread the disease, and that no one gets lost because of failure to return for results.”
Advocates, like the NCSD, have been frustrated with how long it has taken the FDA to grant the rapid-test waiver, but are glad that the agency finally has acted. “NCSD is thrilled that at long last, the FDA has approved a CLIA waiver for a rapid syphilis test. This test is a game-changer in syphilis testing and prevention,” Smith said in a press release.
