The ‘62 Days’ Filmmaker on the Laws That Can Turn a Brain-Dead Pregnant Person Into an ‘Incubator’
In advance of 62 Days' April 15 premier on World Channel's Reel South, Rewire.News spoke with the filmmaker about Marlise Muñoz's case and the impact of pregnancy exclusion laws.
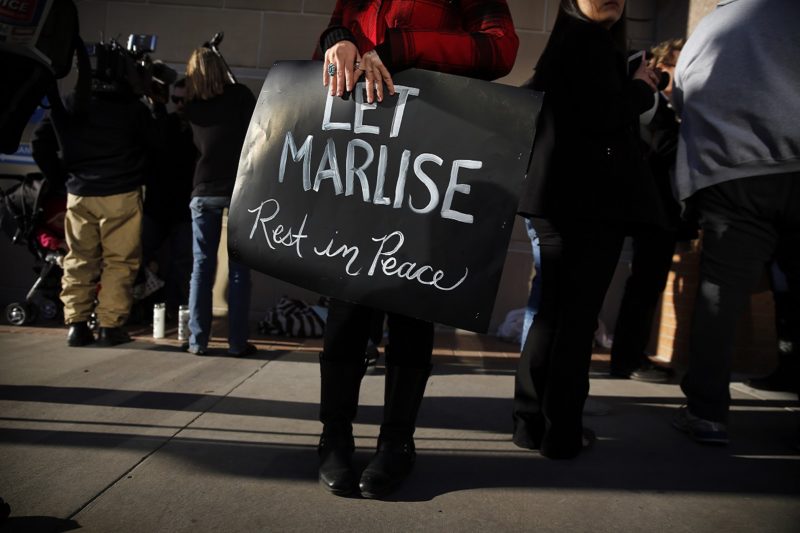
Pregnancy exclusion clauses have been making their way into legislation on states’ advance directives since the 1990s. These laws override any advance directive about end-of-life medical care that a person may have in the case that they are determined to be pregnant. Legislators and other supporters argue such laws are needed to protect the ostensible legal rights of the fetus. However, these exclusions infringe on a pregnant person’s right to refuse unwanted treatment, they can be interpreted to apply to pregnancies where viability would never be a possibility, and, at times, they have been used to turn people into incubators against their stated wishes.
Filmmaker Rebecca Haimowitz tells the story of one such instance in her new documentary 62 Days. Haimowitz, who teaches documentary filmmaking at Rutgers University, previously co-directed and produced Made in India, a feature-length documentary about couples involved with international surrogacy.
62 Days looks at the experience of Marlise Muñoz, a pregnant Texas woman who was declared brain dead after suffering a pulmonary embolism. Due to Texas’ pregnancy exclusion law, and despite the fact that at only 14 weeks pregnant Muñoz was not carrying a medically viable fetus, it took a legal battle for her family to eventually get permission to remove her from mechanical support a full 62 days after her collapse.
In advance of 62 Days’ April 15 premier on World Channel’s Reel South (with subsequent screenings on various PBS stations across the country), Rewire.News had the chance to speak with Haimowitz about the Muñoz family’s experience and their ongoing legal battle to change Texas’ law, the impact of pregnancy exclusion laws, and what people can do if they live in one of the 32 states, according to the film, where such legislation has passed.
Rewire.News: Pregnancy exclusion laws have existed for over 20 years, but a lot of people aren’t familiar with them. Your film really personalizes the impact of such laws. How did you first come across Muñoz’s story?
Rebecca Haimowitz: I discovered the story like a lot of people did, on the news. But there was something about this case that really stuck with me, and I thought there was a lot more to explore.
RN: What was it about it that stuck with you?
RH: It’s hard to imagine a more extreme denial of a woman’s bodily autonomy than putting her dead body on life support to gestate a fetus. It just seems so shocking, and yet it really is the consequence of laws that take rights away from a woman the moment she becomes pregnant. Anyone in this country can determine if they want an advanced directive or a “do not resuscitate” (DNR) order—unless you’re a woman who happens to be pregnant. But so few people know about this.
I think typically when we hear about “fetal protection laws” or “reproductive rights” we automatically assume an abortion debate. But Marlise Muñoz didn’t have an abortion—she died while she was pregnant. And still a law that claims to protect fetal life took the other very personal decision about end-of-life choices [away from her family] and put that in the hands of the state. I recognized that this is a really complicated and deeply personal matter. I wanted to make a film that shows that as well.
RN: Right, I think the end-of-life issue definitely hasn’t been discussed in the same way. I’m sure it isn’t on a lot of people’s radar either.
RH: One of the things about this family is that I think if you had asked them before this happened about their views on reproductive rights, they probably would have said they didn’t have strong thoughts on the issue.
Marlise’s family was not politically motivated, but they swore to honor her wishes and they were determined to do that.
RN: Can you speak a little more about these laws?
RH: In this instance, the law we are referring to is part of the Texas Health and Safety Code, which includes a chapter on advanced directives. An advanced directive is when an individual indicates what should be done if they find themselves in need of mechanical support. Do they want a DNR? Do they want to go off life support? If you don’t have an advanced directive, the choice is typically given to a surrogate decision maker, like a spouse or parent, to decide what’s best.
But if there is a pregnancy exclusion provision, it means that if you are pregnant, whatever choices you and your surrogate made are null and void.
In Marlise’s case, her family agreed 100 percent about what to do. As a paramedic, Marlise had seen many people in this state and had had explicit conversations with her loved ones about what she wanted as a result. Most people, especially most 30-somethings, don’t have those talks. But she did. She had been very clear with her husband and her parents, and still her wishes were ignored because of this little known state law that meant that even though she was brain dead and her pregnancy wasn’t viable—she was only 14 weeks pregnant at the time—the hospital refused to remove her from life support.
RN: What do supporters of this law typically say to justify pregnancy exclusion laws?
RH: They will say that in matters of life and death, we should always err on the side of life. I heard that all the time because I interviewed people who support these laws.
One of the problems I have with that viewpoint is that it’s not medically sound. Just because you can technically use a machine to keep a heart beating does not mean you are valuing a life and often you are drawing out the death process longer.
That was something a lot of doctors talked to me about. The idea that erring on the “side of life” doesn’t promote a life that is viable and obviously doesn’t even respect the life of a woman who has made her choice.
Moreover, these laws makes a big blanket statement about protecting fetal life and don’t look at individual situations. A family may feel differently if their loved one wasn’t technically brain dead but instead in a coma or persistent vegetative state. They may feel differently if her pregnancy was at a more advanced stage. There are a lot of factors that would go into a particular family’s decision. The question is: Do they have a decision to make? Or should the choice be taken from them and put in the hands of the state?
RN: Marlise was from Texas and in the film her family is fighting to change the pregnancy exclusion law there. What is the current status of that fight?
RH: A local judge did eventually rule in favor of the Muñoz family [in their petition to remove Marlise from life support]. But he didn’t rule on the law itself. He ruled on a technicality and the law remains open to judicial interpretation. So in Texas the law hasn’t changed.
The Muñoz family has been working with the American Civil Liberties Union (ACLU) and various legislators to remove the pregnancy exclusion from end-of-life decisions. But it is ongoing.
Texas is only one of 32 states with similar laws. So most states have similar or identical laws on the books—it’s just that few people know that. Since Marlise died, and because of this case, there have been attempts to change the law, on both sides, around the country.
Now there are people trying to make these laws even more explicit and to ensure that laws keep a brain dead woman “alive” if she is pregnant. Louisiana and Nevada ended up passing stricter pregnancy exclusion laws than the ones they had previously had.
RN: If an advanced directive isn’t enough to help someone prevent being kept on life support against their wishes, it there anything else for people to do if they live in states with pregnancy exclusion laws?
RH: You can find out what the law is in your state, and speak to your representatives and let them know that you believe everyone should have the same ability to make end-of-life decisions regardless of their capacity for pregnancy. If you’re not happy with their response, organizations like the ACLU and the National Advocates for Pregnant Women are working on this very issue and can offer action items to help you advocate for change.
RN: What are your hopes for the film?
RH: I hope that, by sharing this story, the film lets people know that these laws exist in a lot of places they might not expect [like in their own state]. And I want them to recognize that real people are affected by these laws.
I hope that we can make some positive changes and put the decision making ability about everything from our reproductive health to our end-of-life care back into the hands of individuals and get it out of the hands of lawmakers and politicians.
This interview has been lightly edited for clarity and length.

