Health Department: Insurers Must Cover All Birth Control Methods
The new guidelines clarify that insurers must cover at least one of each of the 18 FDA-approved methods of birth control, as well as cancer screenings and preventive care for transgender people.
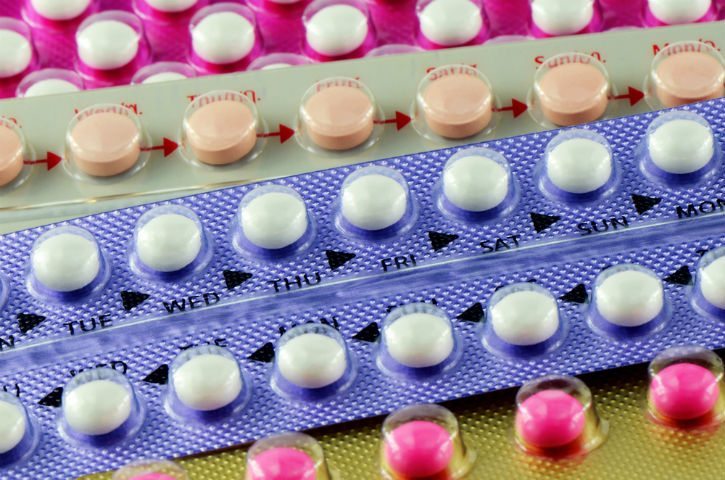
The Department of Health and Human Services (HHS) on Monday issued new guidelines for insurers on birth control coverage, care for transgender people, and other preventive services, in the wake of reports that some insurers are violating the law by not fully covering contraception.
The announcement came less than a week after Senate Democrats sent a letter to HHS Secretary Sylvia Mathews Burwell, citing the “troubling nationwide trend” of insurers denying women coverage, charging them improperly, or giving them inaccurate information.
The new guidelines clarify that insurers must cover, with no cost-sharing, at least one of each of the 18 FDA-approved methods of birth control. That includes methods like the vaginal ring, contraceptive patch, or intrauterine device (IUD).
This was already supposed to be the law under the Affordable Care Act (ACA). But recent reports from the National Women’s Law Center (NWLC) and the Kaiser Family Foundation found that, among other violations, some insurance companies have refused to cover methods like the ring or the patch.
Since the law allowed insurers to use “reasonable medical management” to control costs, some carriers seemed to think they were allowed to exclude these other methods as long as they covered oral contraceptive pills that contained the same hormones.
“Insurance companies have been breaking the law and, today, the Obama Administration underscored that it will not tolerate these violations,” Gretchen Borchelt, NWLC vice president for health and reproductive rights, said in a statement. “It is now absolutely clear that all means all—all unique birth control methods for women must be covered.”
The new guidelines still allow reasonable medical management, but are explicit that it can only be used within each method. That is, an insurer could charge for the non-hormonal IUD to encourage women to use an IUD with hormones, but they couldn’t impose costs on all IUDs simply because they also cover pills that have the same amount of progestin.
Regardless of what insurers choose to cover in their plans, the administration makes clear that they can’t charge extra for any method, brand or generic, pill or other, that the woman’s doctor says is medically appropriate for her. Insurers must have an “easily accessible, transparent, and sufficiently expedient” process to accommodate these kinds of exceptions.
All medical services associated with these birth control methods have to be covered. This is especially important for IUDs, which require a doctor’s appointment for the initial device insertion as well as follow-up appointments. The NWLC found that these follow-up appointments often weren’t covered.
The NWLC also found widespread violations in coverage for maternity care, as well as preventive care like cancer screenings and genetic counseling. The HHS guidelines clarify that insurers have to cover screening and genetic counseling for women whose family history shows an elevated risk of breast or ovarian cancer. And insurers can no longer restrict maternity care for women who are covered by a spouse’s or parent’s insurance.
The birth control issue got the most media attention, but the NWLC also found a widespread lack of needed coverage for transgender people. The new guidelines spell out that insurance companies can’t limit any “sex-specific recommended preventive service” based on a person’s assigned sex at birth, gender identity, or recorded gender, giving the example of mammograms or pap smears for transgender men who still have breast tissue or a cervix.
It’s not clear how the guidelines will affect coverage for transition-related issues like surgery or hormone therapy.
“I’m pleased that with this announcement Secretary Burwell is acting to address these violations as well as others that have become barriers to accessing critical preventive care, especially for those in the transgender community,” Sen. Patty Murray (D-WA), top Democrat on the Senate Health, Education, Labor, and Pensions (HELP) Committee, said in a statement.
